TL;DR:
- Municipal EMS systems face increasing pressure from rising call volumes and limited budgets. EMS consulting improves response times, financial recovery, and system integration through structured assessments and strategic planning. True reform requires interoperability, regional cooperation, and a shift toward community-centered models.
Municipal EMS systems across the United States are under mounting pressure, facing rising call volumes, shrinking budgets, and growing expectations from communities that depend on fast, effective emergency care. Many departments work hard but still miss the mark on response time benchmarks, cost recovery, and clinical outcomes, often because the structural problems are invisible from inside the organization. EMS consulting firms help municipalities achieve faster response times and substantial revenue recovery. This guide walks you through what EMS consulting actually looks like, how experts drive results, and what your municipality can do right now to close critical performance gaps.
Table of Contents
- What is EMS consulting and why does it matter?
- Core EMS consulting methodologies: How experts drive results
- Performance measurement and national benchmarks in EMS consulting
- Navigating complexities: Rural, urban, and edge-case EMS challenges
- Financial, policy, and integration considerations in EMS consulting
- Perspective: The biggest gap in municipal EMS reform — and how to close it
- Next steps: Optimize your municipal EMS system with expert guidance
- Frequently asked questions
Key Takeaways
| Point | Details |
|---|---|
| Expert impact | EMS consulting delivers measurable improvements in response times, efficiency, and revenue recovery for municipalities. |
| Strategic methodology | Consultants follow proven frameworks involving stakeholder engagement, goal setting, and KPI monitoring. |
| Benchmark-driven results | Consultants help systems meet or exceed national benchmarks using evidence-based analytics and continuous monitoring. |
| Tailored solutions | Expert guidance adapts strategies to address rural, urban, and special-case EMS challenges for better outcomes. |
| Integration focus | Transformational EMS improvement requires integrated data, public health partnerships, and modern policy approaches. |
What is EMS consulting and why does it matter?
At its core, EMS consulting is the practice of engaging outside experts to evaluate, redesign, and strengthen emergency medical services systems. Unlike internal reviews that often confirm existing assumptions, consulting engagements bring structured objectivity and cross-jurisdictional experience that internal teams rarely have access to. This outside perspective is precisely where measurable change begins.
A well-scoped consulting engagement typically covers a broad range of services, including:
- Operational assessment: Analyzing unit deployment, call-to-door intervals, System Status Management (SSM), and crew scheduling
- Financial analysis: Reviewing billing practices, reimbursement rates, payer mix optimization, and cost-per-transport ratios
- Strategic planning: Developing multi-year service delivery roadmaps aligned with community growth and budget realities
- Regulatory and compliance review: Ensuring adherence to state licensure, CMS (Centers for Medicare and Medicaid Services) requirements, and HIPAA standards
- Leadership development: Building the internal capacity to sustain improvement after the engagement ends
EMS consulting firms like PCG, Fitch and Associates, Matrix Consulting Group, and Public Administration Associates provide specialized services to U.S. municipalities and fire/EMS departments, each bringing distinct methodologies but a shared commitment to measurable outcomes.
The return on investment is well-documented. One nationally recognized firm recovered $18.5 million in revenue for 16 EMS providers by correcting billing gaps and updating reimbursement coding practices. For municipal leaders managing constrained budgets, that kind of recovery is not a luxury. It is operational survival.
“Effective EMS consulting does not just find problems — it builds the internal capability to prevent them from recurring.”
For a broader overview of EMS consulting and the advantages of EMS consulting for public safety outcomes, the evidence consistently points to improved response performance, better financial health, and stronger community trust. A well-structured strategy guide for EMS can serve as a starting point before a full engagement begins.
Core EMS consulting methodologies: How experts drive results
Knowing what EMS consulting offers is useful. Understanding how consultants actually do the work is what allows you to evaluate a firm’s approach and hold them accountable for results.
Most high-performing consulting engagements follow a structured, phased methodology. Consultants use a 5-step strategic model: assess operations, engage stakeholders, set SMART goals, allocate resources via RACI matrices, and monitor and adapt over time. Each phase builds on the last, and skipping any of them tends to produce short-lived improvements.
Here is how the process typically unfolds:
- Initial diagnostic: Review historical call data, CAD (Computer-Aided Dispatch) records, response time reports, and financial statements
- Stakeholder engagement: Conduct structured interviews with crew members, supervisors, medical directors, and municipal finance staff
- KPI gap analysis: Compare current performance against national benchmarks on response times, call volumes, ALS/BLS (Advanced Life Support/Basic Life Support) utilization, and clinical outcomes
- Strategy development: Draft SMART (Specific, Measurable, Achievable, Relevant, Time-bound) goals with RACI (Responsible, Accountable, Consulted, Informed) matrices for accountability
- Implementation and monitoring: Deploy performance dashboards, conduct follow-up audits, and refine strategy based on real-time data
In-house approach vs. EMS consulting firm approach
| Factor | In-house team | EMS consulting firm |
|---|---|---|
| Objectivity | Limited by internal bias | High; cross-jurisdictional view |
| Data access | Local only | National benchmarks and peer data |
| Speed of diagnosis | Slower; competing priorities | Focused, structured timeline |
| Cost recovery expertise | Generalist knowledge | Specialized billing/reimbursement skills |
| Sustainability of change | Variable | Structured handoff and training |
PCG serves 550+ providers nationwide with detailed operational studies, demonstrating how scalable this methodology is across diverse municipal contexts. Operational audits in EMS form the backbone of any credible engagement, while a documented EMS strategic planning process ensures findings translate into lasting system improvements.
Pro Tip: Do not underestimate phase-by-phase stakeholder buy-in. Resistance to change is the most common reason consulting recommendations stall at the report stage. Build engagement into every phase, not just the beginning.
Performance measurement and national benchmarks in EMS consulting
You cannot improve what you do not measure. This principle sits at the heart of any credible EMS consulting engagement, and it is where many municipal systems discover their most significant gaps.

EMS benchmarking data from national organizations like ESO and ImageTrend gives consultants a reliable reference point for evaluating where your system stands relative to peer agencies across the country. These benchmarks cover clinical performance, operational efficiency, and resource utilization, providing a multi-dimensional view of system health.
Key KPIs every municipal EMS system should track include:
- Response time percentiles: 90th percentile response time for Priority 1 calls, measured from dispatch to arrival
- Airway management success rates: First-attempt intubation success and supraglottic device utilization
- Stroke assessment completion rates: Percent of suspected stroke patients receiving a validated assessment tool like the Cincinnati Prehospital Stroke Scale
- Lights and sirens (L&S) utilization rate: Overuse of emergency mode increases crew risk without proportionate benefit
- Return of spontaneous circulation (ROSC) rates: Outcome measure for cardiac arrest response quality
- Unit hour utilization (UHU): Efficiency ratio of productive time vs. available unit hours
Consultants use EMS performance optimization strategies to map your current data against these benchmarks and identify where performance gaps carry the highest risk, whether clinical, financial, or operational. System design consulting best practices then inform how resources are repositioned to close those gaps. For a detailed look, the municipal EMS guide outlines how to align your system design with these measurement frameworks from the ground up.
Navigating complexities: Rural, urban, and edge-case EMS challenges
Not every EMS system faces the same challenges, and the consulting approach that works for a dense urban fire department will not translate directly to a rural volunteer service covering 400 square miles. Effective consultants recognize this and tailor their recommendations accordingly.
Rural systems, particularly those serving populations under 25,000, face acute staffing constraints, longer transport distances to definitive care, and heavy reliance on volunteer crews. Urban systems contend with high call volume density, demand surges during events, and complex mutual aid coordination. Tradeoffs between rural, urban, and special EMS scenarios are often best addressed through regional cooperation and innovative deployment models.
Common edge-case consulting scenarios include:
- Regionalization feasibility studies: Evaluating whether merging two or more small EMS services creates better coverage and cost efficiency
- Mass casualty incident (MCI) planning: Developing triage, transport, and hospital notification protocols for low-frequency, high-impact events
- Civil unrest and disaster surge planning: Coordinating with law enforcement, emergency management, and public health for integrated response
- Volunteer retention and recruitment strategy: Addressing the staffing crisis facing rural volunteer agencies
- Air medical integration: Determining when and how to incorporate helicopter EMS (HEMS) into rural response protocols
National thought leadership calls for EMS to evolve beyond a transport-only model, particularly in underfunded or underserved areas where the system must serve a broader community health function. Selecting the right deployment models for municipalities and investing in municipal response consulting gives leaders the framework to make these decisions with confidence rather than guesswork.
Pro Tip: Leverage existing mutual aid agreements and regional CAD data early in the planning process. Cross-jurisdictional data reveals demand patterns that single-agency data will always underrepresent.
Financial, policy, and integration considerations in EMS consulting
EMS is chronically underfunded relative to fire and police, and this disparity is not simply a budget problem. It reflects a structural misalignment in how emergency services are categorized, reimbursed, and politically prioritized at the municipal level.
Underfunding, outdated reimbursement structures, and siloed public safety systems consistently limit EMS efficacy across the country. Best practice responses include reimbursement optimization and closer integration with the broader healthcare system. The actionable steps for municipal leaders in this space include:
- Audit current billing and coding practices to identify reimbursement gaps under Medicare, Medicaid, and commercial payers
- Explore alternative funding streams such as federal grants, public health partnerships, and community paramedicine (CP) program reimbursement
- Engage state legislators on updated EMS reimbursement schedules that reflect current operational costs
- Integrate EMS data with hospital systems to create bidirectional clinical feedback loops that improve patient outcomes and support value-based care models
- Adopt a community health role by deploying EMS resources for preventive care, frequent 911 user intervention, and post-discharge follow-up
“The shift from reactive 911 response to an integrated public health model is not optional for systems that want long-term financial sustainability. It is the only viable path forward.”
Working with reimbursement consultants for EMS ensures your billing infrastructure captures every dollar your crews have earned. Pairing that with a solid public policy guide for EMS positions your municipality to advocate effectively at both the state and federal level. EMS funding research continues to surface new models that forward-thinking municipalities are already implementing.
Perspective: The biggest gap in municipal EMS reform — and how to close it
Here is what most municipal leaders do not hear until it is too late: incremental improvements rarely produce transformational results. New ambulances, upgraded radio systems, and revised protocols all matter. But without genuine system integration, they are isolated upgrades that leave the underlying dysfunction intact.
In our experience, the most common reason consulting projects stall is that municipalities treat recommendations as a checklist rather than a connected system change. They adopt one best practice here, adjust one policy there, and then wonder why response performance has not shifted meaningfully.
The real gap is interoperability. Most U.S. EMS systems lag in interoperable data, real-time analytics, and coordinated hospital-EMS handoffs, which prolongs avoidable inefficiency across the entire care continuum. Until your CAD talks to your hospital’s admission system and your field crews receive clinical feedback on their patients, you are operating with significant blind spots.
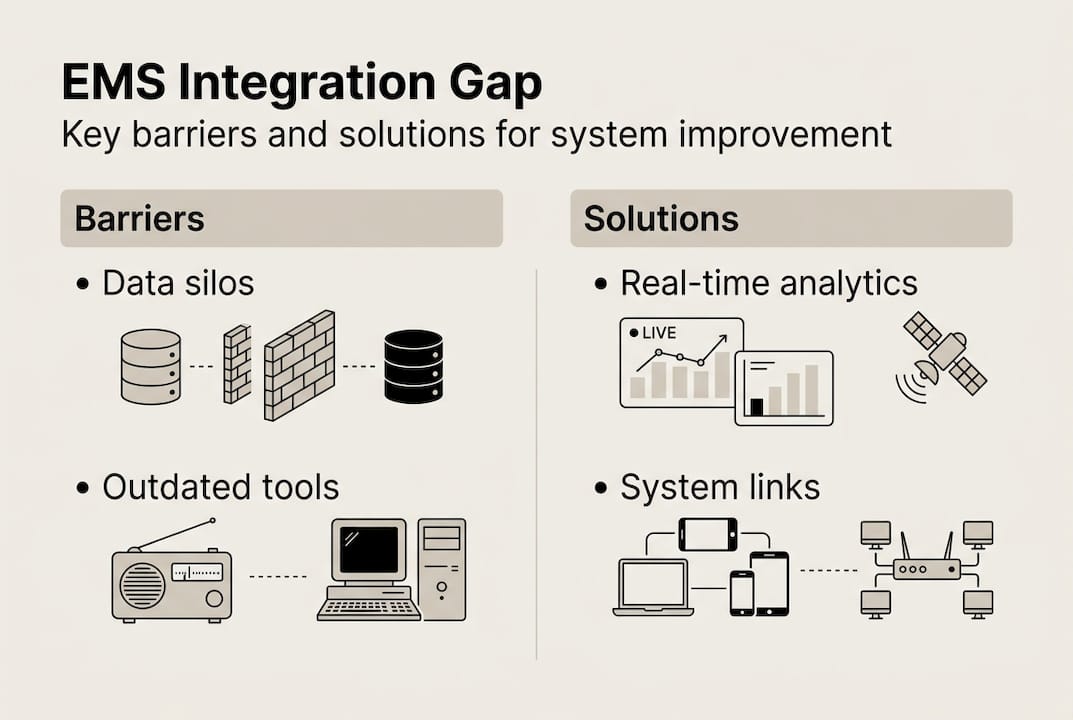
We challenge you to prioritize true system integration over headline upgrades. A long-term municipal EMS strategy built on data interoperability and coordinated care delivery will outlast any single equipment purchase or staffing adjustment by years.
Next steps: Optimize your municipal EMS system with expert guidance
The operational, financial, and policy knowledge covered in this guide points toward one clear conclusion: expert consulting is the most efficient lever available to municipal leaders seeking measurable public safety improvements. Whether you are starting with a performance gap analysis or ready for a full system redesign, the path forward begins with a structured, evidence-based assessment.
We encourage you to explore our municipal EMS strategy guide for a practical framework you can act on immediately. When you are ready for deeper support, our EMS system design consulting services give your municipality a partner with the expertise to drive real, lasting change. Contact our consulting experts today to start the conversation.
Frequently asked questions
What services do EMS consulting firms provide?
EMS consulting firms provide operational analysis, financial reviews, staffing optimization, response planning, and strategic master planning. Services are typically tailored to the specific needs and resource profile of each municipality.
How do EMS consultants improve response times?
Consultants use operational assessments, data analytics, and resource deployment strategies to pinpoint delays and implement faster response solutions. Predictive analytics applied to 911 call data have reduced EMS response times by as much as 12% in documented urban deployments.
What benchmarks do EMS consultants use for performance?
Consultants rely on national benchmarks from ESO and ImageTrend reports, measuring response times, clinical procedures, and system-level metrics. These standards allow direct comparison between your system and peer agencies nationally.
How do consultants account for challenges in rural EMS systems?
They recommend regional cooperation strategies, customized deployment models, and mutual aid frameworks designed for communities with limited staffing or geographic barriers. Volunteer retention and air medical integration are also common focus areas.
What is the future direction for EMS as advised by consulting leaders?
Leading experts advocate for integrated, patient-centered EMS models that partner with public health agencies to improve outcomes. NHTSA and global EMS thought leaders point toward community paramedicine, data interoperability, and coordinated hospital partnerships as the defining priorities for the next decade.







